
Specialized Clinics, Programs and Services
Baycrest’s clinics and programs offer care, assessments and support for older adults and their families. Some focus on medical care, while others provide therapy, education and wellbeing support.

Adult Day Programs
The Baycrest Community Day Centre for Seniors provides supervised part-day programs for older adults who live outside of Baycrest.
Learn More
Behavioural Support for Seniors Program
The Behavioural Support for Seniors Program helps older adults with cognitive problems and their families manage difficult behaviours.
Learn More
Centre for Neurology and Behavioural Support
The Pamela and Paul Austin Centre for Neurology and Behavioural Support treats a wide range of neurological and brain conditions.
Learn More
Day Treatment Centre
The Saul and Rae Saltzman Day Treatment Centre offers outpatient programs to help older adults with complex medical conditions improve their quality of life.
Learn More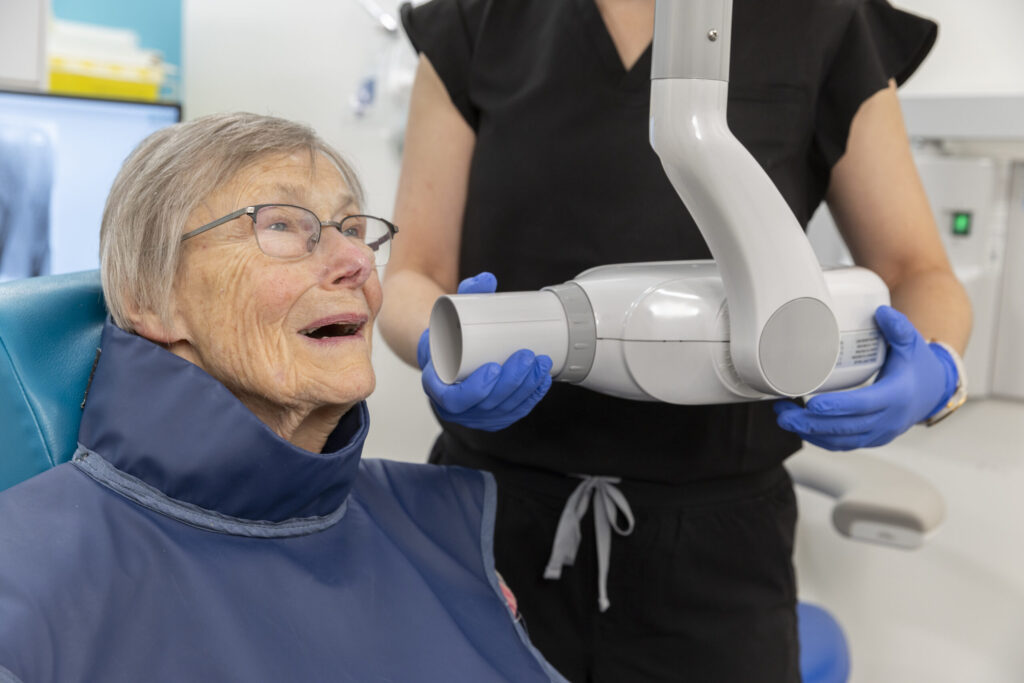
Dental Centre
The Alpha Omega Dental Centre offers a full range of dental services with a focus on care for older adults.
Learn More
Falls Prevention Program
The Falls Prevention Program offers classes that teach older adults how to maintain their strength and balance to prevent falls.
Learn More
Fees Swallowing Test
The FEES Swallowing Test clinic performs endoscopic tests to assess swallowing problems.
Learn More
Foot Care Clinic
The Foot Care Clinic offers a wide range of treatments to promote foot health.
Learn More
Geriatric Assessment Clinic
The Geriatric Assessment Clinic offers specialized assessments for older adults with significant health challenges.
Learn More
Geriatric General Neurology Clinic
The General Neurology Clinic diagnoses and treats a wide range of neurologic conditions in older adults.
Learn More
Geriatric Psychiatry Community Service
The Geriatric Psychiatry Community Service (GPCS) provides mental health services for homebound older adults.
Learn More
Goal Management Training™
Goal Management Training™ provides small group training to help people with diagnosed executive functioning deficits.
Learn More
Hearing Services
Baycrest Hearing Services offers hearing tests and custom solutions for hearing loss.
Learn More
Holocaust Resource Program
The Holocaust Resource Program runs support groups and socials for Holocaust survivors and their families.
Learn More
Integrated Community Care Team
The Integrated Community Care Team provides health care to homebound older adults in their own homes.
Learn More
Interprofessional Primary Care Team
The Interprofessional Primary Care Team (IPCT) helps adult patients of any age with chronic health conditions and complex medical needs.
Learn More
Learning the Ropes for Living with MCI ®
Learning the Ropes for Living with MCI® provides small group training to help people with mild cognitive impairment and memory loss.
Learn More
Memory Clinic
The Sam and Ida Ross Memory Clinic helps help diagnose and treat memory loss and other cognitive issues.
Learn More
Memory Link®
Memory Link® teaches people with moderate-to-severe memory problems to use technology to help with memory functioning.
Learn More
Memory and Aging Program ®
The Memory and Aging Program® gives older adults practical solutions for improving their memory.
Learn More
Mental Health Services
The Centre for Mental Health assesses and treats older adults living with mental health problems.
Learn More
Movement Disorders Clinic
The Movement Disorders Clinic provides specialized care for people with movement disorders like Parkinson’s disease.
Learn More
Neuropsychology and Cognitive Health
The Neuropsychology and Cognitive Health program offers a range of services for clients with neurological and memory concerns.
Learn More
Psychiatric Day Hospital
The Psychiatric Day Hospital runs outpatient programs for older adults with mood or anxiety disorders.
Learn More
Spasticity Management Clinic
The Spasticity Management Clinic helps people with neurological disorders manage muscle stiffness.
Learn More
The Virtual Behavioural Medicine Program
Virtual Behavioural Medicine offers virtual neuropsychiatric support to health-care providers and families managing challenging and aggressive behaviours in people living with dementia.
Learn More
Voice Treatment Clinic
The Voice Treatment Clinic helps people with Parkinson’s disease strengthen their voice.
Learn More